Why Spinal Instability Goes Missed Without Proper Imaging
Spinal instability is one of the most commonly missed causes of chronic pain, especially in patients who have been injured in a car accident. Many people are told their scans are “normal,” yet they continue to experience neck pain, back pain, headaches, or a feeling that their spine is weak or unreliable. In many of these cases, the problem is not a lack of movement—it is too much uncontrolled movement.
Without proper imaging, spinal instability often goes undiagnosed, leaving patients trapped in cycles of temporary relief and recurring symptoms.
What Spinal Instability Really Means
Spinal instability occurs when the structures that stabilize the spine—primarily ligaments and joint capsules—can no longer properly control motion between vertebrae. The spine may still move freely, but it moves beyond normal physiological limits.
Instability can lead to:
- Excessive joint motion
- Abnormal stress on discs
- Muscle overactivation and fatigue
- Irritation of nerves or the spinal cord
Unlike fractures, instability does not show up as an obvious injury. It is a functional problem, not a gross structural failure.
Why Car Accidents Commonly Cause Instability
Motor vehicle collisions expose the spine to rapid acceleration and deceleration forces. Ligaments are particularly vulnerable because they are designed to limit motion—not absorb sudden force.
After a car accident:
- Ligaments may stretch or partially tear
- Normal spinal curves may be altered
- Joint mechanics change instantly
These changes can persist even after pain decreases. Over time, repeated stress on unstable segments can lead to chronic symptoms and early degeneration.
Why Standard Exams Often Miss Instability
Traditional physical exams are limited in their ability to detect instability. Muscle strength and range of motion may appear normal, especially in patients who have adapted to their injury.
Standard imaging also has limitations. Neutral-position X-rays and routine MRI scans may fail to show:
- Excessive motion between segments
- Dynamic instability that appears only during movement
- Subtle ligament injury
As a result, patients may be told nothing is wrong—even when instability is driving their symptoms.
The Importance of Functional Imaging
To identify instability, imaging must evaluate how the spine behaves under movement or load. This is where functional imaging becomes essential.
Examples include:
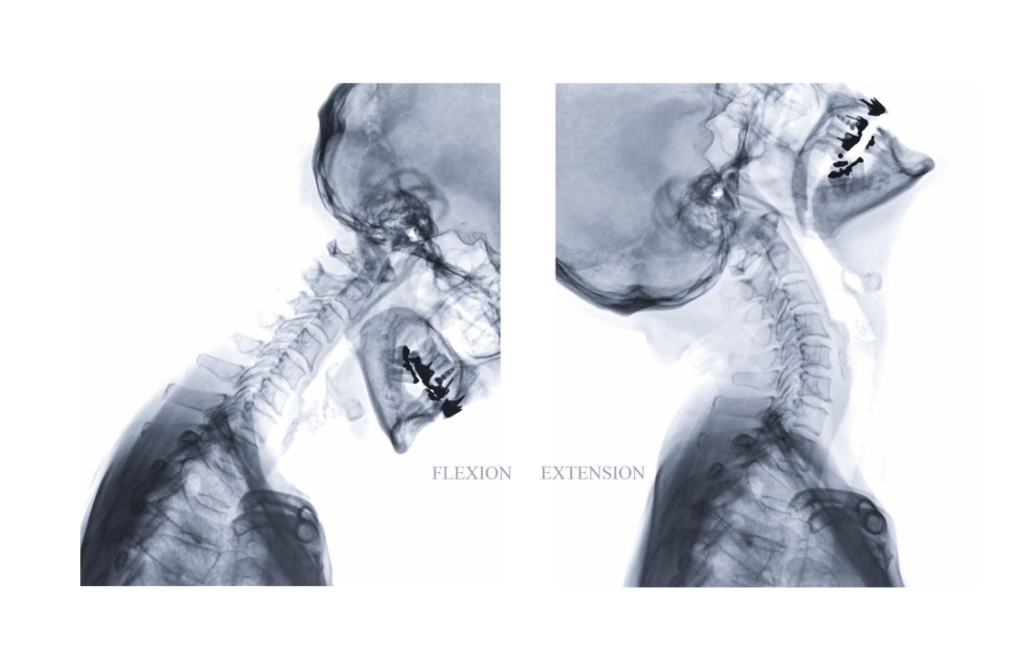
- Flexion/extension X-rays
- Flexion/extension MRI
- Specialized upper cervical imaging when indicated
These studies assess whether vertebrae move excessively relative to one another, revealing instability that static images cannot capture.
Upper Cervical Instability: A Commonly Overlooked Area
The upper cervical spine (C0–C2) relies heavily on ligaments for stability and houses critical neurological structures. Trauma to this region can produce symptoms such as:
- Persistent headaches
- Dizziness or balance issues
- Neck weakness or fatigue
- Neurological sensitivity
Standard imaging protocols may not adequately visualize upper cervical ligaments. Specialized imaging techniques are often required to assess stability in this region accurately.
Why Missing Instability Affects Recovery
When instability goes unrecognized, care may focus on increasing motion in an already unstable spine. This can:
- Provide short-term relief
- Increase ligament stress
- Worsen long-term instability
- Accelerate degeneration
Patients may cycle through treatments without lasting improvement because the core problem is never addressed.
Identifying instability changes everything about treatment strategy.
How Proper Imaging Changes the Care Plan
Once instability is identified, care shifts toward:
- Stabilization rather than aggressive mobilization
- Structural correction to improve alignment
- Controlled rehabilitation progression
- Long-term mechanical support
This approach protects injured tissues and reduces the likelihood of chronic flare-ups.
The Elevation Health Perspective
At Elevation Health, spinal instability is approached as a biomechanical diagnosis, not a vague explanation.
Imaging decisions are guided by:
- Trauma history
- Persistent or recurrent symptoms
- Clinical signs of instability
When appropriate, functional and specialized imaging is used to ensure that excessive motion is not overlooked—particularly in patients injured in car accidents.
Patients are educated on how instability affects their spine and why corrective strategies are necessary for long-term recovery.
Long-Term Consequences of Undiagnosed Instability
If spinal instability remains untreated, it often leads to:
- Progressive joint degeneration
- Disc damage
- Chronic pain syndromes
- Reduced tolerance for physical activity
These changes may not be immediate, but they accumulate over time.
Seeing the Problem Others Miss
Spinal instability does not always announce itself clearly. It hides behind “normal” scans and temporary symptom relief. Without proper imaging, it remains invisible.
Functional and specialized imaging reveal how the spine truly behaves—allowing care to move beyond guesswork and toward precision-based correction.
Stability Is the Foundation of Healing
For the spine to heal, it must be stable. Identifying instability is the first step toward restoring normal function and preventing future breakdown.
Proper imaging makes that possible.

